
Justice and Mental Health Collaboration Act
October 17, 2013Individuals with mental illnesses are significantly overrepresented in the prison and jail population. State and local governments are increasingly finding the need for greater collaboration between criminal justice, juvenile justice, and mental health and substance abuse treatment systems to better allocate resources across systems, increase connections to needed services, and reduce recidivism.
The Mentally Ill Offender Treatment and Crime Reduction Act (MIOTCRA) created the Justice and Mental Health Collaboration Program (JMHCP) to help states and counties design and implement collaborative efforts between criminal justice and mental health systems. The Justice and Mental Health Collaboration Act (JMHCA) of 2013 reauthorizes the successful MIOTCRA and extends the JMHCP for five years.
NAPO is a strong supporter of the JMHCP, which helps criminal justice and mental health agencies work collaboratively towards better outcomes. The JMHCP can help law enforcement agencies across the United States in their responsibilities in assisting those, and dealing with citizens with mental health issues. NAPO has worked closely with key staffers for the JMHCA's sponsor, Senator Franken, to ensure the passage of this legislation during the 113th Congress.
The Wall Street Journal article at the end of this report, The New Asylums: Jails Swell with Mentally Ill, illustrates the importance of passing the JMHCA.
If you have any questions about this legislation, please contact Melissa Nee at: mnee@napo.org.
Source:
Fields, Gary, and Erica Phillips. "The New Asylums: Jails Swell With Mentally Ill." Wall Street Journal. WSG, 25 Sept. 2013. Web. 1 Oct. 2013..
The New Asylums: Jails Swell With Mentally Ill
America's Jails Face Growing Need to Provide Mental-Health Treatment
By: Gary Fields and Erica E. Phillip

Patrick T. Fallon for The Wall Street Journal
An inmate looked out from his locked cell door at Twin Towers Correctional Facility.
CHICAGO—The sound of clanging steel doors and agitated voices in the Cook County Jail bullpen was deafening. Amid the din, Robert Miller, who would turn 19 the next day, wept quietly. Anger and sullenness were common here. Uncontrolled crying was a sign of a bigger problem.
Mr. Miller was being held on a drug-possession charge and was waiting for his day in court. But his anguish caught the attention of a woman on the other side of the bars. Elli Petacque Montgomery, the jail's chief clinical social worker, listened as Mr. Miller spoke and shuddered. The teenager, who disputes the drug charge, said he had tried in vain to get help for his disabling episodes. Twice, he said, he had attempted suicide.
Battling Mental Illness in Lockup

Philip Scott Andrews for The Wall Street Journal
A man held on to fencing while awaiting processing at Cook County Jail.
Ms. Montgomery scribbled notes on a clipboard. At the jail, she routinely sees people with conditions ranging from severe depression to schizophrenia.
"It's going to be a long day," she said.
America's lockups are its new asylums. After scores of state mental institutions were closed beginning in the 1970s, few alternatives materialized. Many of the afflicted wound up on the streets, where, untreated, they became more vulnerable to joblessness, drug abuse and crime.
The country's three biggest jail systems—Cook County, in Illinois; Los Angeles County; and New York City—are on the front lines. With more than 11,000 prisoners under treatment on any given day, they represent by far the largest mental-health treatment facilities in the country. By comparison, the three largest state-run mental hospitals have a combined 4,000 beds.
Put another way, the number of mentally ill prisoners the three facilities handle daily is equal to 28% of all beds in the nation's 213 state psychiatric hospitals, according to the National Association of State Mental Health Program Directors Research Institute Inc.
"In every city and state I have visited, the jails have become the de facto mental institutions," says Esteban Gonzalez, president of the American Jail Association, an organization for jail employees.
Correctional systems define mental illness differently. Generally, the term is used to describe prisoners who require medication for serious issues ranging from major depressive disorders to schizophrenia and bipolar disorders. Also included are inmates with diagnoses that warrant overnight stays in a mental hospital or who demonstrate serious functional impairment.
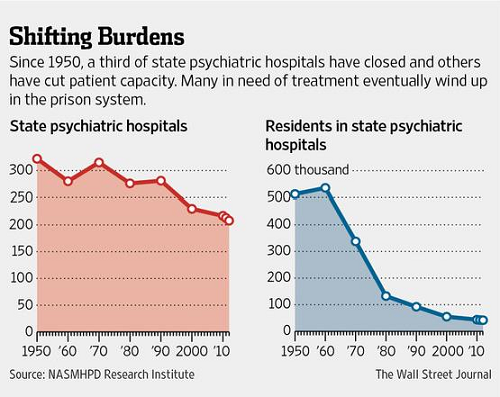
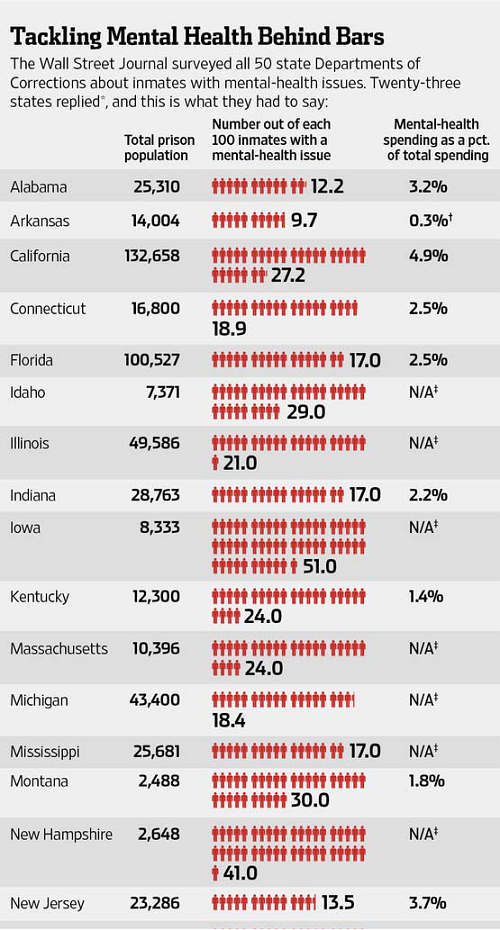
To get a snapshot of how the U.S. is grappling with such an explosive societal issue, The Wall Street Journal surveyed all 50 states about issues of mental health within their prison populations. Of the 22 states that provided detailed responses, their mental-health patient ratios ranged from one in 10 inmates to one in two. Inmates in all 23 responding states account for 55% of the prisoners in the U.S. under state jurisdiction.
In Oregon, the trend is particularly acute. Officials there estimate that half the state's 14,000 prison inmates suffer from some type of mental-health issue.
Several states with large inmate populations, like Michigan and Illinois, reported to the Journal that about 8% to 10% of their inmates suffered from serious mental illnesses, such as schizophrenia. Smaller states, like Montana, said as many as 15% of their inmates suffered from serious mental illness.
Roughly 5% of all adult Americans suffer from a serious mental illness, according to a 2012 report by a division of the U.S. Department of Health and Human Services.
Caring for such distressed inmates is costly. National Alliance on Mental Illness, one of the leading advocacy research groups, estimates that prisoners with mental illness cost the nation $9 billion annually.
Other challenges are evident. In Los Angeles, for example, the U.S. Department of Justice found in 1997 that mentally ill inmates were abused and endured conditions that violated their federal civil rights.
Earlier this month the DOJ sent a letter to L.A. officials saying that despite some apparent progress, there is "a growing number" of mentally ill inmates housed in general population quarters at Men's Central Jail, as well as a "recent increase in suicides."
Assistant Los Angeles County Sheriff Terri McDonald said the growing population of mentally ill inmates "certainly strains the system." She said they would continue to work with DOJ officials "and we welcome their thoughts."
Some facilities have attempted to cope by hiring psychiatric staff and retraining prison officers. Few, however, claim to be adequately equipped to handle some of the nation's most mentally frail. A seeming revolving door compounds the problem: Upon their release, the mentally ill tend to find scant resources and often quickly fall back into the system, says Mr. Gonzalez.
Even in some areas that have seen reductions in the general inmate population, the mentally ill constitute a growing share of correctional space.
For example, New York City's total prison population has fallen to 11,500, down from 13,576 in 2005. Yet the number of mentally ill prisoners has risen, to 4,300 from 3,319, says Dora Schriro, commissioner of corrections for the city. That means the city's percentage of mentally ill prisoners grew from 24% to 37%.
The picture echoes the past. Two centuries ago, reformers were disturbed to find large numbers of the mentally ill in jails, paving the way for the development of state-run institutions. In the 1950s and 1960s, complaints about abuses, advances in medication and a push to give the patients more independence led to another change, this time toward community settings. The weaknesses of that concept—a lack of facilities, barriers created by privacy laws and tightened local and state funding—has brought the picture full circle.
"Society was horrified to warehouse people in state hospitals, but we have no problem with warehousing them in jails and prisons," says Thomas Dart, sheriff of Cook County.
At Cook County, mental-health staffers like Ms. Montgomery function much like air-traffic controllers—routing troubled prisoners to the appropriate unit, inside or outside the jail, for care. On the day of Mr. Miller's tearful outburst, the shuffle was in full swing.
Those with mental problems could possibly avoid a jail term in favor of outside treatment. "Gentlemen, we can help you [in court] if you give us the information we're looking for" said one of Ms. Montgomery's three staff members. The announcement prompted prisoners to line up to speak to one of the women with clipboards.
The questions focus on possible problems: "Have you ever been hospitalized for a mental illness? Does anyone in your family suffer from mental illness?"
Ms. Montgomery is responsible for evaluating the jail's new arrivals. On that July morning, eight of the first 10 prisoners, she determined, suffered from some type of mental illness. The information would later be referred to judges, prosecutors and defense lawyers to help determine how a prisoner might be handled across the system.
Mr. Miller, who had been sitting in a corner, weeping, said he had not previously been diagnosed as mentally ill. But during his assessment, he said he had suffered from major depression for years. Help wasn't easy to find.
He said he had been hospitalized for several days after a suicide attempt but was released once stabilized. A spokeswoman at the hospital said privacy regulations prevented her from discussing Mr. Miller's specific case.
"I didn't know who else to ask," said Mr. Miller, who has a preliminary court date next month.
During the past year, Chicago shut six of 12 city-run mental-health clinics to save money. The recent closure of a state mental hospital has left the South Side with no such facility.
In an interview with the Journal, Mr. Miller said that he had used heroin in the past to "make my pain and problems go away but it always comes back."
Many of the prisoners' stories sounded similar—they had been living on the streets, using alcohol and illegal drugs. Several had attempted suicide, primarily by overdosing.
The inmates' conditions include severe depression, bipolar disorders and schizophrenia, said Gary Kaniuk, the psychologist who runs mental-health services in one area of the jail.
"Mental health is a reality of what we're going to house here." Assistant sheriff in Los Angeles
Sheriff Dart visits the dormitories regularly. During a recent tour, prisoners rushed over to him. Several were about to be released and wanted his help in finding a place where they could stay and get treatment for their illnesses.
After hearing out several prisoners, Mr. Dart said he was most troubled by the case of Steven Dorsey. Mr. Dorsey, 48, was a part-time worker at a janitorial supply company, but his hours had dried up in recent months, and he lost his job. Mr. Dorsey, who said he had been diagnosed as bipolar and schizophrenic, had felt lucky to be placed in a group home. He had to leave, though, after Medicaid turned him down for benefits, he said.
He ended up living on the streets, occasionally scrounging in dumpsters for food scraps.
The group home didn't respond to calls for comment. His former employer, Daniel Marquez, said he had tried to help Mr. Dorsey on a temporary basis. He called his situation, including his mental-health issues, "tragic."
"I didn't have a way of eating or sleeping," says Mr. Dorsey. Voices told him to "steal what you need." He ended up in jail after allegedly lifting a sandwich and a toothbrush from a convenience store. A sheriff's spokesman said he was charged with retail theft under $300.
The sheriff confirmed Mr. Dorsey's account. "These are not crimes of a criminal mastermind," Mr. Dart says.
Prisoners sometimes commit what are considered nuisance crimes—but they do them repeatedly, landing them in jail. They get booked, get treatment and then are released with a limited supply of medication. Often, they run out of the drugs before they are able to be placed in a treatment facility, Mr. Dart says. They then often commit the same offenses that landed them in jail in the first place.
The rapid influx of the mentally ill is creating new fractures in the system. Because inmates with highly acute mental illness often need to be housed individually, more than 300 beds at the Twin Towers Correctional Facility in Los Angeles go unused, while many in the general population bunk in overcrowded dorms and dayrooms.
About 400 of the jail's male prisoners are under intense supervision. They are housed in semicircular pods originally built for general-population inmates. Each individual cell has a glass door that opens onto the pod's common area. Because their actions are often unpredictable, the inmates are handcuffed to tables in the common room during therapy sessions.
"The goal here is to stabilize them, so they can be moved to a lower level of care," says Jeffrey Marsh, a supervising psychiatrist in the jail.
Assistant Sheriff McDonald, who oversees the jail system, notes that the highest recidivism rates are among mentally ill inmates. Ms. McDonald is among several county officials pushing for a new jail facility designed specifically for mental-health and drug-abuse treatment. Such a project would cost between $1.3 billion and $1.6 billion, according to an independent study commissioned by the county.
"Mental health is a reality of what we're going to house here," Ms. McDonald said. A jail that can adequately treat those offenders, she added, "is a better investment."
Currently, the budget for the jail's mental-health services is about $35 million a year. That covers a staff of 300, which includes 37 psychiatrists and 50 social workers.
Across the country, other prison officials are grappling for solutions to a many-pronged problem.
In Oregon, the job of prison officers has drastically evolved in recent years, says Jana Russell, director of mental-health services for the Oregon Department of Corrections.
The state is training officers how to best respond to a mentally ill inmate. One tool the state has adopted, which has been used by other departments, is a code system that signals how seriously ill an inmate might be, without violating medical privacy laws. The department also trains the officers on what symptoms to look for, since they are often the first to spot changes in behavior, Ms. Russell said.
Oregon's neighbor to the north has created a prison within a prison at the Monroe Correctional Complex in Monroe, Wash. In total, the system has about 750 mental-health beds for the most seriously ill, although it has thousands of inmates with mental-health problems.
Monroe has a designated area to handle mentally ill inmates: the special offenders unit, which resembles a hospital. Gone is the smell of sweat and the palpable tension more typically found in the general prison population. All public places are encased in glass, allowing staff to watch inmates closely.
Deborah Franek, one of the supervisors in the special unit, said one resident sculpted his feces. Another would "bite his fingers off a joint at a time," she said.
In the closed observation area, three inmates were under 24-hour watch. One, in a straitjacket, had attempted suicide while detained. Two others were in the midst of major psychotic breakdowns.
Karie Rainer, director of Mental Health Services for the system, used to work at the state mental hospital, which has slowly been cutting beds. Recently, she has noticed a marked trend: Several patients she once saw at the hospital are now in the special unit at Monroe.
The days of focusing on security alone are gone for prisons, says Bruce Gage, chief of psychiatry to the Washington Department of Corrections. "We're finding sicker and sicker people all the time" who have to be treated for their mental illnesses. Prisons "can't say no to the mentally ill. They have to solve the problem."